(I wrote this Wednesday, so all time references are from that perspective).
Has it already been four days since Hope was born? Has it only been four days?
Life in the NICU is certainly a new experience. So far it’s been good though, other than trying to juggle being a mom to Ella who is at home and a mom to Hope who is at the hospital. I’m only two days in to commuting to the NICU from home, so I guess I shouldn’t be too hard on myself for not figuring out a good balance yet. I’ve found that it works for me to be at the hospital in the morning, go home for lunch and getting Ella down for a nap, rest a little, and then come back to the hospital in the late afternoon for part of the evening. But I realized Tuesday that that means I’m only with Ella during her worst hours of the day: meals that preceed sleep (when we’re both tired), and then the falling asleep window of time (which is sometimes unfortunately long). No wonder she’s been having such a rough time adjusting to Mommy being home the past two days. She wants me to do everything, even things that other people are doing for themselves (like making tea), and she loses it when for any reason I don’t do the thing she wants me to do. So today I slept in to forego the need for a nap, stayed home for the morning to spend time with Ella, and went to the hospital from about 1:30-6:30, and that worked much better for all of us. Ella actually fell asleep on her own in her crib for both naptime and bedtime after I sat at her bedside for a little while and pumped (she’s fascinated by my pumping).
As for Hope, she’s doing wonderfully. She was 3lbs 1oz at birth, which different doctors and nurses have happily pronounced “A good size!” and “Average size” for her gestational age. Other doctors and nurses have said “Well she won’t be a heavyweight” and “She’s a peanut!” and “Why is she so little? Did they say what caused her to be IUGR?” (IUGR = intrauterine growth restriction. It means for some reason a baby isn’t growing adequately in utero. I/she had a diagnosis of “mild IUGR” while I was in the hospital based on sonogram measurements of her growth). Anyway… 3lbs is bigger than I expected her to be since she had been 2lbs 10oz only a week before, and she looks bigger than I expected. And she looks healthy, just small.
When Hope first came up to the NICU she was placed on a radiant warmer which is an open bed with a heater above her. Pros of the radiant warmer are that the medical staff (and parents!) have easy access to the baby to get her situated that first day and take care of any issues that arise, and it easily keeps her nice and toasty. Cons are that since it’s radiant heat it causes babies to lose fluids pretty rapidly and therefore lose weight as well. So they wanted to get her into an “isolette” as soon as she was stable. That happened Sunday morning. The isolette is an enclosed, double-walled thick plastic incubator with six little portholes around the sides. The long side walls also open all the way to allow easier access when the doctors and nurses need it, and for getting the baby in and out as necessary. It’s also heated, but it’s a different kind of heat than the open bed she was on. The isolette looks much scarier than the radiant warmer; the first time we walked in and saw her in it I thought “Wow, now she really looks like a preemie.” It looks so much more like what I think people picture when they imagine a baby in intensive care. But I know it’s actually a step in the right direction.
Hope started getting feedings of my pumped breastmilk through a “gavage tube” (that goes down her throat to her stomach) on Saturday, starting at 4mls (almost a teaspoon! So tiny!), and she gets milk every three hours. She’s also on a continuous IV of lipids and fluids that include proteins, vitamins, amino acids, and other good stuff she needs (Idk what else…). That IV currently goes into her umbilical site and is called a “UVC.” That’s the easiest way for them to give fluids and draw blood when necessary to avoid sticking her with needles repeatedly. They can only use that site for about five days though, so it will be coming out soon and she’ll probably get a PICC line instead. Starting Sunday, they started increasing her milk feeds by 2mls every 12 hours. She’s currently up to 14mls per feeding. I think the doctor said the goal is 30mls (1 ounce) per feed by 7-10 days old, at which point they’ll discontinue the IV nutrients and she’ll be on “full feeds” status. However, they can’t increase her feeds too rapidly because she’s little and they don’t want to overwhelm or damage her stomach by stretching it too quickly. So they do a bunch of things before every feeding to make sure she’s tolerating the increased amount. They measure the circumference of her belly to make sure she digested enough of the milk (I forget what the threshold is), so her belly would be bigger if she had milk leftover in it. They also suction the gavage tube to see how much milk, if any, is left in her belly. As long as it’s less than 40% of what she was given at the last feeding, they’re happy.
If I’m here during feedings I get to do “oral care” when she gets her milk. Oral care is when I get a drop or two of my breastmilk on a tiny swab and rub it inside her cheeks and across her tongue. The proteins from the milk are absorbed into her cheek tissue, it cleans her mouth, and it teaches her to associate the taste of breastmilk with the feeling of a full belly. The first couple of times I got to do it I used the little swab, but then they ran out of them, and apparently the manufacturer isn’t making them anymore. So the nurse 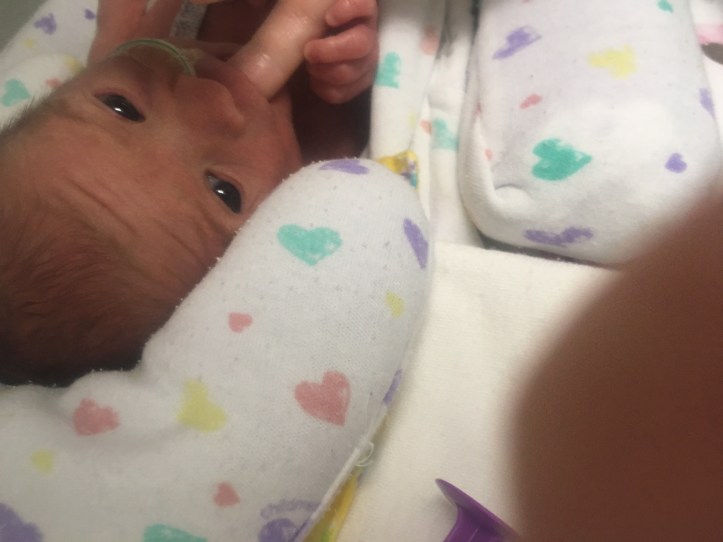 yesterday and today just had me use my pinky, and that was so cool! To get to feel her tiny little mouth and tongue and give her the chance to suck on my finger if she wanted to was much more personal than swabbing her mouth.
yesterday and today just had me use my pinky, and that was so cool! To get to feel her tiny little mouth and tongue and give her the chance to suck on my finger if she wanted to was much more personal than swabbing her mouth.
Within minutes of being born the neonatologist who was in the room intubated Hope to help her breathe. She cried and breathed on her own when she was born, but at such a young age babies may not be reliable to keep breathing on their own. Throughout Saturday they weaned the number of breaths that the ventilator was giving her through the ET tube (that’s the one in her throat for breathing) until Sunday morning at 12:30am when they were able to switch to a nasal respirator instead. 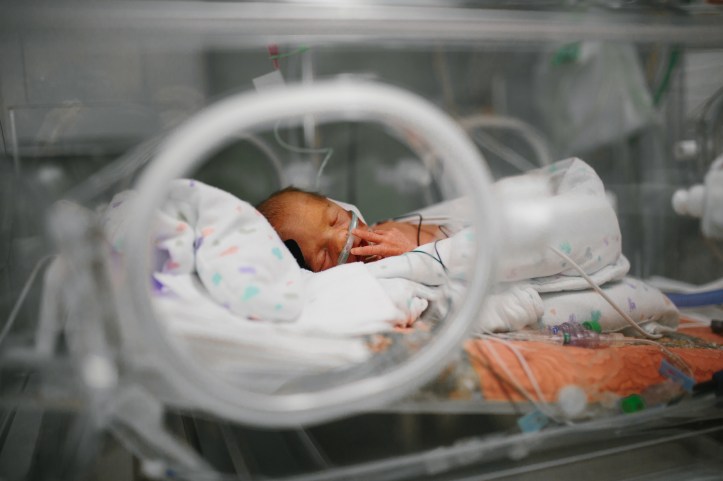
They repeated the process of weaning how many breaths the machine gave her, and Monday just before noon they removed that and let her breathe room air on her own. She has tolerated that beautifully; they haven’t had to give her assistance breathing with any devices that would be a step down from the ventilator (options I know of would be a nasal cannula or oxygen hood, there may be others). To make sure her breathing is effectively healthy, they check the amount of different gasses in her blood a couple of times per day. So far all of her numbers have been great.
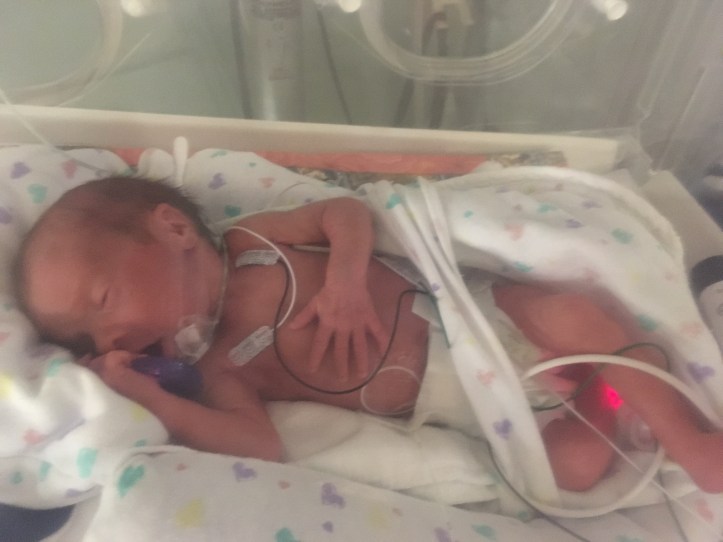
Because of the UVC and the lack of knowledge about her brain health the first few days, we weren’t able to hold Hope. So when we visit Hope we do “containment holding” to mimic the womb environment by placing our hands firmly but gently on the top of her head, holding her legs folded in toward her bum, or holding her arms folded across her chest. It helps keep her from startling (which wastes her energy) and generally makes her feel more comfortable. It also lets her get to know our touch and scent and gives us a way to participate in her care and comfort.
She had her head ultrasound Tuesday morning, and a nurse practitioner told me if the results were normal I could probably hold her. I was shocked to hear that, and super excited of course, because I thought the reason to not be able to hold her was the UVC. Later in the morning a doctor came in with the good news that her head ultrasound looked good, so I got to hold her for the first time yesterday afternoon! We did Kangaroo Care, which is where you hold the baby chest to chest straight on your skin and cover both parent and baby up with warm blankets. She snuggled right in on my chest with her feet tucked up in froggy position and drifted off into a deep sleep. We were both so content the whole time. It was awesome. I’m amazed and so pleased that even though she spends the majority of her time without me right now she already seems to know me. It’s such a relief every time I successfully comfort her when she gets upset in her isolette; despite the separation, she seems to know her mama :o)
She’ll have another head ultrasound at one month old to assess for developmental delays. The neonatologist who told me that said the risk is very low for her because she made it to 30 weeks, didn’t have an infection, and isn’t sick.
For now we can only Kangaroo once per day, so Nathanael got to hold her for the first time today! I love how excited he was about it :o) Sometimes I forget that dads have feelings about their babies, too 😛
(All the nice photos in this post are thanks to my sweet sister-in-law Hannah at Hannah Grace Photography).








She looks beautiful. Photos make her look big. My Michael was 9# 7 oz when born and to think she is just 1/3 of what he was. I realize she is very small as he was very big! Congrats again!
LikeLike